You moved to one of the sunniest places on Earth, and somehow your vitamin D levels came back low. Your doctor seemed surprised. You felt confused. After all, the sun here is relentless, the kind that bleaches car interiors and makes you squint even with sunglasses. How could you possibly be deficient in the sunshine vitamin?
Here’s the thing: This article contains affiliate links. See our affiliate disclosure for details. The Gulf region has some of the highest rates of vitamin D deficiency globally, with studies showing 60-80% of residents have insufficient levels. It’s a paradox that catches nearly everyone off guard. The abundance of sunshine doesn’t translate to adequate vitamin D when your lifestyle necessarily revolves around avoiding that very sun.
Medically reviewed by Dr. Layla Hassan, Trichologist. If you’ve noticed increased hair shedding, persistent fatigue, or slower wound healing since moving to a sun-heavy climate, vitamin D deficiency might be the hidden factor. Research suggests this deficiency is particularly common among expat women in the Gulf, where cultural norms, extreme heat, and modern indoor lifestyles create a perfect storm for inadequate vitamin D synthesis.
Key Takeaways
• Living in sunny climates doesn’t guarantee adequate vitamin D due to sun avoidance behaviors, indoor lifestyles, and protective clothing requirements
• 60-80% of Gulf residents show vitamin D deficiency despite year-round intense sunlight, with women and those with darker skin particularly affected
• Vitamin D deficiency can contribute to hair loss by changeing follicle cycling and stem cell function, independent of other nutritional factors
• Glass windows, sunscreen above SPF 15, and clothing block the UVB rays necessary for vitamin D synthesis, even in direct sunlight
• Supplementation of 1,000-2,000 IU daily may be necessary for most Gulf residents, with higher doses required for those with confirmed deficiency
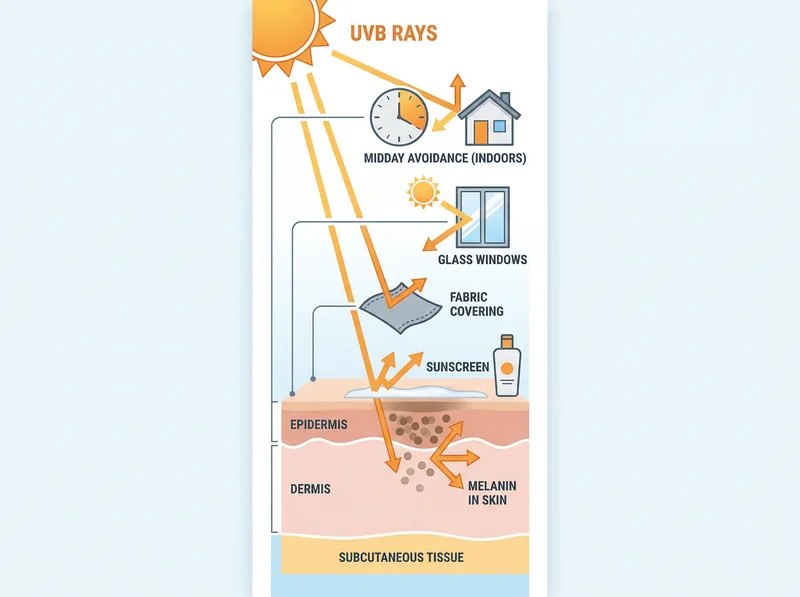 Multiple environmental and behavioral factors prevent vitamin D synthesis even in sun-rich regions.
Multiple environmental and behavioral factors prevent vitamin D synthesis even in sun-rich regions.
The Sunshine Paradox: Why Sun Doesn’t Equal Vitamin D
The assumption seems logical. More sun equals more vitamin D. But research published in the Journal of Steroid Biochemistry shows that environmental vitamin D availability and actual vitamin D status are completely different things. You can live at 25°N latitude with 340 sunny days per year and still be profoundly deficient.
The disconnect happens because vitamin D synthesis requires a specific set of conditions that rarely align in sun-heavy climates. You need direct UVB exposure to bare skin, at the right time of day, for a sufficient duration. But when temperatures regularly exceed 40°C and the UV index hits extreme levels, every instinct and cultural norm pushes you indoors or into protective clothing.
Consider the typical day in the Gulf region. You wake up, get ready indoors, walk to your car in covered parking, drive to work with tinted windows, spend eight hours in an air-conditioned office, drive home, and maybe venture out after sunset when UVB rays are minimal. Even weekend outdoor activities happen early morning or evening to avoid the brutal midday heat. Your sun exposure is either filtered through glass or happens when the sun angle is too low for vitamin D production.
Add in the necessary sun protection, and the paradox deepens. The American Academy of Dermatology recommends daily sunscreen use in high-UV environments. SPF 30 blocks about 97% of UVB rays. The long sleeves, wide-brimmed hats, and UV-protective clothing that prevent sun damage also prevent vitamin D synthesis. You’re caught between skin cancer risk and nutritional deficiency.
Why Gulf Residents Are Particularly Vulnerable
The Gulf region presents unique risk factors that compound the sunshine paradox. A study in the Journal of Nutrition examining vitamin D status across the GCC found that despite abundant sunshine, prevalence of deficiency ranged from 60-83% depending on the country and demographic group studied. Women and those with darker skin pigmentation showed the highest deficiency rates.
Melanin acts as a natural sunscreen, which is protective against UV damage but reduces vitamin D synthesis efficiency. Research suggests that individuals with darker skin may need 3-5 times longer sun exposure to produce the same amount of vitamin D as those with lighter skin. In a climate where even brief sun exposure feels punishing, this extended exposure requirement becomes practically impossible to meet.
Cultural dress codes add another layer. Many women in the region wear clothing that covers most of their body, leaving minimal skin exposed to sunlight. Even those who don’t follow traditional dress codes often choose long sleeves and full-coverage clothing simply because it’s more comfortable in extreme heat. The fabric provides cooling through air circulation while blocking the UVB rays needed for vitamin D production.
The indoor lifestyle is nearly universal. Homes, offices, shopping centers, and even outdoor spaces are air-conditioned or designed to minimize heat exposure. You can live your entire life moving between climate-controlled bubbles, with outdoor time limited to the few tolerable hours after sunset. This isn’t laziness or preference. It’s adaptation to an environment where summer temperatures make prolonged outdoor exposure genuinely dangerous.
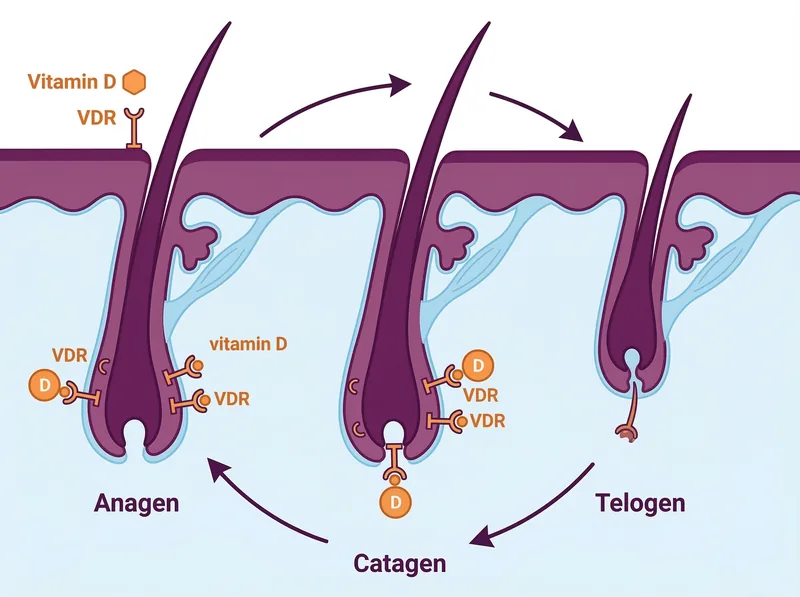 Vitamin D plays a crucial role in hair follicle stem cell activation and the growth phase of the hair cycle.
Vitamin D plays a crucial role in hair follicle stem cell activation and the growth phase of the hair cycle.
The Hidden Cost: What Vitamin D Deficiency Does to Your Body
Vitamin D isn’t just about bone health, though that’s certainly important. This hormone (it’s technically not a vitamin) has receptors in nearly every tissue in your body, including your hair follicles, immune cells, and cardiovascular system. When you’re deficient, the effects cascade across multiple systems.
Mayo Clinic lists fatigue, bone pain, muscle weakness, and mood changes as common symptoms of deficiency. But many people don’t recognize these as vitamin D related because they develop gradually and feel like normal responses to stress or aging. You might chalk up your persistent tiredness to jet lag, work stress, or the climate adjustment rather than a nutritional deficiency.
The immune system impact is particularly relevant. Vitamin D plays a crucial role in immune regulation, and deficiency is associated with increased susceptibility to infections and slower wound healing. If you’ve noticed you’re catching every cold that goes around the office, or that minor cuts take weeks to heal completely, vitamin D status is worth investigating.
For women, the reproductive health implications are significant. Research indicates that vitamin D deficiency may affect menstrual regularity, fertility, and pregnancy outcomes. The connection isn’t fully understood, but vitamin D receptors are present in reproductive tissues, and the hormone appears to play a role in hormone regulation and egg quality.
Vitamin D and Hair Loss: The Follicle Connection
If you’re experiencing increased hair shedding or thinning since moving to a sun-heavy climate, vitamin D deficiency might be a contributing factor. Research published in Dermatology and Therapy shows that vitamin D plays a critical role in hair follicle cycling, and deficiency can change the normal growth phase.
Hair follicles contain vitamin D receptors, and these receptors are essential for maintaining the stem cells that regenerate hair. When vitamin D levels are insufficient, follicles may prematurely enter the resting phase or fail to transition back to active growth. This doesn’t cause the dramatic hair loss you’d see with alopecia areata, but rather a gradual thinning and increased daily shedding that’s easy to dismiss as stress or aging.
The connection becomes more complex when you factor in the environmental stressors common in dry, hard water climates. Mineral buildup on the scalp can interfere with nutrient delivery to follicles, and if those follicles are already compromised by vitamin D deficiency, the combined effect can accelerate thinning. Using a chelating shampoo like Regrowth+ to remove mineral deposits while addressing vitamin D deficiency through supplementation creates a more supportive environment for hair growth.
The research on vitamin D supplementation for hair loss is still emerging, but several studies show promise. Women with telogen effluvium (excessive shedding) who corrected vitamin D deficiency showed improvement in hair density and reduction in shedding over 3-6 months. It’s not a miracle cure, but it’s a foundational factor that shouldn’t be overlooked.
Testing and Optimal Levels: What the Numbers Mean
The standard test for vitamin D status measures 25-hydroxyvitamin D, or 25(OH)D, in your blood. This is the storage form of vitamin D and the most accurate indicator of your overall status. But what constitutes adequate levels is surprisingly controversial among medical professionals.
The National Institutes of Health defines deficiency as below 20 ng/mL (50 nmol/L), insufficiency as 20-30 ng/mL, and sufficiency as 30 ng/mL or higher. However, many functional medicine practitioners and endocrinologists argue that optimal levels for health are higher, in the 40-60 ng/mL range. Some research suggests that levels below 30 ng/mL may be insufficient for optimal immune function and cellular health.
If you’re getting tested in the Gulf region, don’t be surprised if your doctor seems unconcerned about levels in the 20-25 ng/mL range. The clinical definition of deficiency is conservative, focused on preventing rickets and osteomalacia rather than improving overall health. If you’re experiencing symptoms like fatigue, hair loss, or frequent illness, it’s worth discussing supplementation even if your levels technically fall above the deficiency threshold.
Testing frequency matters too. Vitamin D status can fluctuate based on sun exposure, supplementation, and even season (though seasonal variation is less pronounced in year-round sunny climates). If you start supplementing, retest after 3 months to ensure you’re reaching target levels without overshooting into toxicity, which can occur above 100 ng/mL.
Supplementation Strategy: Getting It Right
Supplementing vitamin D in a sun-heavy climate feels counterintuitive, but it’s often necessary. The question isn’t whether to supplement, but how much and what form. Vitamin D3 (cholecalciferol) is generally preferred over D2 (ergocalciferol) because it’s more effective at raising and maintaining blood levels.
For general maintenance in the Gulf region, research suggests 1,000-2,000 IU daily is appropriate for most adults. If you’re starting from a deficient state (below 20 ng/mL), your doctor may recommend a higher loading dose of 4,000-5,000 IU daily for several weeks, then dropping to maintenance levels once you reach target range. Some practitioners use weekly high-dose supplementation (50,000 IU once per week) for severe deficiency, though daily dosing is generally better tolerated.
Timing and co-factors matter. Vitamin D is fat-soluble, so take it with a meal containing healthy fats for optimal absorption. Magnesium is required for vitamin D metabolism, and many people in the Gulf region are also deficient in magnesium due to poor dietary intake and mineral-depleted water. Consider supplementing both, or choose a vitamin D supplement that includes magnesium and vitamin K2, which work synergistically.
Don’t assume that because you’re taking a multivitamin, you’re covered. Most standard multivitamins contain only 400-800 IU of vitamin D, which is insufficient for correcting deficiency in a sun-avoidance lifestyle. Check your supplement labels and calculate your total daily intake from all sources.
Can You Get Enough from Food Alone?
The short answer is: probably not. Very few foods naturally contain vitamin D in significant amounts. Fatty fish like salmon, mackerel, and sardines are the best sources, providing 400-600 IU per 3-ounce serving. Egg yolks contain about 40 IU each. Fortified foods like milk, orange juice, and cereals add some vitamin D, but you’d need to consume large quantities to meet daily requirements through diet alone.
In the Gulf region, dietary vitamin D intake tends to be lower than in Western countries due to different food fortification practices and dietary patterns. Many traditional Middle Eastern and South Asian foods are not naturally high in vitamin D, and fortification of staple foods is less common. If you’re following a plant-based diet, the challenge is even greater, as the few plant sources of vitamin D (mushrooms exposed to UV light) are not widely available.
That said, improving dietary vitamin D intake is still worthwhile as part of a complete approach. Aim to include fatty fish 2-3 times per week, choose fortified dairy or plant milk, and don’t skip the egg yolks. Every bit helps, even if it’s not sufficient on its own.
Safe Sun Exposure: Finding the Balance
Is it possible to get adequate vitamin D from sun exposure in the Gulf without risking skin damage? The answer is complicated. UVB rays are strongest between 10am and 2pm, which is precisely when dermatologists tell you to avoid sun exposure. But it’s also when vitamin D synthesis is most efficient.
Some research suggests that 10-15 minutes of midday sun exposure to arms and legs, without sunscreen, 2-3 times per week may be sufficient for lighter-skinned individuals to maintain adequate vitamin D levels. For those with darker skin, this time may need to extend to 30-40 minutes. But in a climate where the UV index regularly reaches 10+ (extreme), even brief unprotected exposure carries skin cancer risk.
The practical compromise for most people is strategic, limited sun exposure combined with supplementation. Perhaps you expose your arms during a brief morning walk before applying sunscreen for the day. Or you spend 15 minutes in your garden before the heat becomes unbearable. These small exposures won’t fully meet your vitamin D needs, but they contribute while minimizing skin damage risk.
Glass blocks UVB rays, so sitting by a sunny window or driving in your car won’t help with vitamin D synthesis, even though you feel the warmth. You need direct exposure to the sky, which makes balcony or outdoor space access valuable for those living in apartments.
References
- Vitamin D and the skin: An update for dermatologists - Journal of Steroid Biochemistry and Molecular Biology
- Vitamin D status across the Gulf Cooperation Council countries - Journal of Nutrition
- The Role of Vitamin D in Hair Follicle Biology and Hair Loss - Dermatology and Therapy
- Vitamin D Deficiency: Symptoms and Causes - Mayo Clinic
- Vitamin D Fact Sheet for Health Professionals - National Institutes of Health
