You’ve tried the supplements. You’ve switched shampoos. You’re doing everything right for your hair, but you’re still waking up exhausted and watching more strands collect in the shower drain each week. Here’s what most women don’t realize: the missing piece might not be in your bathroom cabinet. It’s a mineral deficiency that affects nearly 70% of women, changes your sleep architecture, improves your cortisol, and quietly sabotages hair growth at the follicle level.
Magnesium is involved in over 300 enzymatic reactions in your body, including the ones that regulate your stress response, support deep sleep, and maintain healthy hair follicle function. When you’re deficient, which most women living in high-stress environments are, your body enters a state of chronic physiological tension. Your sleep becomes fragmented. Your cortisol stays improved. And your hair follicles, highly sensitive to stress hormones, shift prematurely into the shedding phase. This article contains affiliate links. See our affiliate disclosure for details.
The connection between magnesium, sleep quality, and hair health isn’t speculative. Research published in the Journal of Research in Medical Sciences found that magnesium supplementation significantly improved sleep quality and reduced cortisol levels in adults with insomnia. A separate study in Nutrients demonstrated that magnesium deficiency impairs hair follicle cycling and contributes to telogen effluvium, the most common form of stress-related hair loss in women. The mechanism is clear: poor sleep improves cortisol, improved cortisol changes hair growth, and magnesium deficiency underlies both problems.
If you’re an expat living in the Gulf, the risk is even higher. Desalinated water lacks the mineral content of natural water sources, meaning you’re not getting incidental magnesium from tap water the way you would in other regions. Add chronic heat exposure, which increases magnesium loss through sweat, and high-stress professional environments, and you have a perfect storm for deficiency. Here’s how to identify it, test for it, supplement correctly, and support both your sleep and your hair recovery.
Why Magnesium Deficiency Is So Common in Women
Magnesium deficiency, clinically termed hypomagnesemia, affects an estimated 60-70% of women in developed countries, according to data from the National Institutes of Health. But the standard American diet, high in processed foods and low in magnesium-rich whole foods, is only part of the story. Women face additional depletion factors that men don’t.
Hormonal fluctuations during the menstrual cycle increase magnesium excretion. Research shows that magnesium levels drop significantly during the luteal phase, which is why many women experience worse sleep, more anxiety, and increased muscle tension in the week before their period. Oral contraceptives further deplete magnesium stores, as do common medications including proton pump inhibitors (PPIs) for acid reflux and diuretics for blood pressure.
Chronic stress is the most significant drain. When your body perceives stress, it mobilizes magnesium from your cells to fuel the fight-or-flight response. In short bursts, this is adaptive. But in the context of chronic work stress, sleep deprivation, or major life transitions like relocation, your magnesium stores become chronically depleted. And because magnesium is required to regulate the stress response itself, you end up in a vicious cycle: stress depletes magnesium, low magnesium amplifies your stress response, and the cycle continues.
In the Gulf region specifically, environmental factors compound the problem. Desalinated water, which is the primary drinking water source across the GCC, contains virtually no magnesium compared to natural groundwater. A study published in Science of the Total Environment found that populations relying on desalinated water had significantly lower dietary magnesium intake and higher rates of cardiovascular and metabolic issues linked to magnesium insufficiency. You’re not getting the 20-30mg of magnesium per liter that you’d get from natural mineral water, and most women don’t compensate through diet.
 Magnesium deficiency symptoms often overlap and compound each other, creating a cycle of poor sleep and physical stress.
Magnesium deficiency symptoms often overlap and compound each other, creating a cycle of poor sleep and physical stress.
The Sleep-Cortisol-Hair Loss Connection
Your hair doesn’t fall out because you had one bad night of sleep. It falls out because chronic sleep changeion keeps your cortisol improved, and improved cortisol directly damages hair follicles. The mechanism is well-established in dermatological research.
Hair follicles cycle through three phases: anagen (growth), catagen (transition), and telogen (rest/shedding). Under normal conditions, about 85-90% of your hair is in the active growth phase at any given time. But cortisol, your primary stress hormone, forces follicles to exit the growth phase prematurely and enter the shedding phase. A study in PLOS One found that chronic improvion of cortisol shortens the anagen phase and prolongs telogen, resulting in diffuse hair thinning across the scalp.
This is where magnesium becomes critical. Magnesium acts as a natural antagonist to cortisol. It regulates the hypothalamic-pituitary-adrenal (HPA) axis, the system that controls your stress response, and it’s required for the production of GABA, the neurotransmitter that promotes relaxation and deep sleep. When you’re magnesium-deficient, your HPA axis becomes dysregulated. Your cortisol stays improved even when there’s no acute stressor, your sleep architecture deteriorates (you spend less time in deep, restorative sleep stages), and your hair follicles pay the price.
The research is unambiguous. A 2012 study in the Journal of Research in Medical Sciences found that magnesium supplementation (500mg daily for eight weeks) significantly improved sleep quality, increased sleep time, and reduced early morning awakening in elderly adults with insomnia. More importantly, it reduced serum cortisol levels, suggesting that magnesium’s sleep benefits are mediated through stress hormone regulation. For women experiencing telogen effluvium, the most common stress-related hair loss pattern, addressing magnesium deficiency is foundational.
How to Know If You’re Deficient
Standard blood tests won’t catch magnesium deficiency. Serum magnesium, the test most doctors order, only reflects about 1% of your body’s total magnesium stores. Most of your magnesium is stored in bones and soft tissues, not circulating in your blood. You can have severely depleted cellular magnesium and still show normal serum levels.
The most accurate test is the RBC magnesium test (red blood cell magnesium), which measures intracellular magnesium levels. This test is more expensive and not routinely ordered, but it’s worth requesting if you have multiple symptoms of deficiency. A normal RBC magnesium level is 4.0-6.5 mg/dL. Anything below 4.0 indicates deficiency, and levels below 3.5 are considered severe.
Symptomatically, magnesium deficiency presents as a constellation of issues that women often attribute to other causes. The most common signs include difficulty falling asleep or staying asleep, frequent waking between 2-4am (when cortisol naturally dips and magnesium-dependent neurotransmitters should promote deep sleep), muscle cramps or twitches (especially in the calves or feet), eyelid twitching, chronic fatigue despite adequate sleep, anxiety or irritability, brain fog, and diffuse hair thinning without a clear pattern.
If you’re experiencing three or more of these symptoms, especially if you’re also dealing with chronic stress or recent relocation, magnesium deficiency is highly likely. The good news is that it’s one of the most straightforward nutritional deficiencies to correct, and the benefits for sleep and hair health are often noticeable within two to four weeks of consistent supplementation.
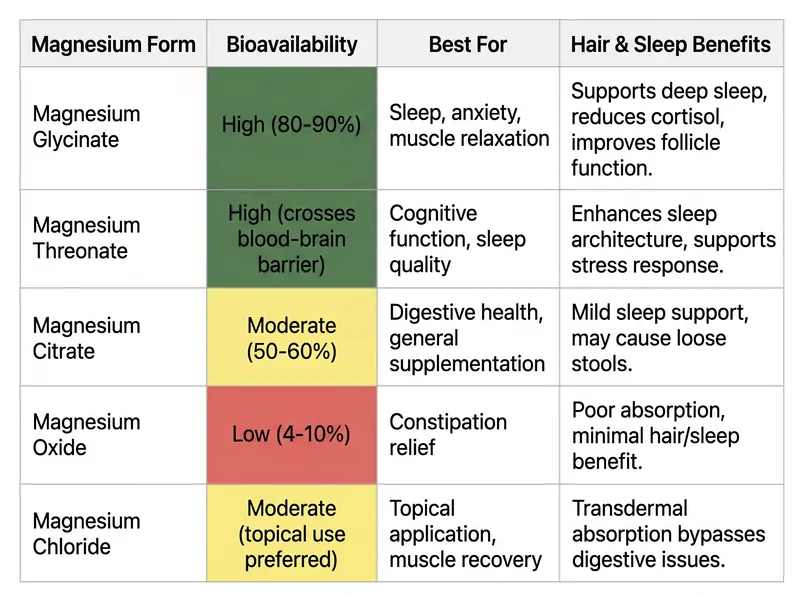 Not all magnesium supplements are equal. Glycinate and threonate offer the best absorption and targeted benefits for sleep and hair.
Not all magnesium supplements are equal. Glycinate and threonate offer the best absorption and targeted benefits for sleep and hair.
Which Form of Magnesium Actually Works
Not all magnesium supplements are created equal. The form matters significantly because different forms have different bioavailability (how much your body actually absorbs) and different affinities for specific tissues. If you’re taking magnesium oxide, the most common form in cheap multivitamins, you’re absorbing less than 10% of what you’re swallowing.
For sleep and hair health, the two most effective forms are magnesium glycinate and magnesium threonate. Magnesium glycinate is magnesium bound to the amino acid glycine, which is itself a calming neurotransmitter. This form has high bioavailability (80-90% absorption), doesn’t cause digestive upset or loose stools, and has been shown in clinical trials to improve sleep quality and reduce anxiety. It’s the gold standard for women who need magnesium for stress reduction and sleep support.
Magnesium threonate (also called magnesium L-threonate) is the only form that efficiently crosses the blood-brain barrier, making it particularly effective for cognitive function and sleep architecture. A study published in Neuropharmacology found that magnesium threonate increased brain magnesium levels by 15% and improved both short-term and long-term memory in animal models. For women dealing with brain fog, poor sleep quality, and stress-related hair loss, this form offers targeted benefits.
Avoid magnesium oxide and magnesium sulfate (Epsom salts taken orally) for supplementation. These forms have poor absorption and primarily act as laxatives. Magnesium citrate has moderate absorption and is useful for constipation, but it’s not the best choice if your primary goal is sleep and hair support. Topical magnesium (magnesium chloride oil) can be helpful as an adjunct, especially for muscle tension, but it shouldn’t replace oral supplementation because you can’t reliably achieve therapeutic blood levels through skin absorption alone.
 Whole food sources of magnesium provide cofactors that enhance absorption, but most women still need supplementation to reach optimal levels.
Whole food sources of magnesium provide cofactors that enhance absorption, but most women still need supplementation to reach optimal levels.
Dosing, Timing, and What to Expect
The recommended dietary allowance (RDA) for magnesium is 310-320mg per day for women aged 19-30 and 320-360mg for women over 30, according to the National Institutes of Health. But these values are set to prevent frank deficiency, not to improve function. For therapeutic purposes, especially for sleep and stress management, most functional medicine practitioners recommend 400-600mg of elemental magnesium per day, divided into two doses.
Timing matters. Magnesium taken in the evening, 30-60 minutes before bed, has the most pronounced effect on sleep quality. This is when you want the calming, muscle-relaxing, cortisol-lowering effects to kick in. If you’re taking a higher dose (500-600mg), split it into a morning dose (200mg) and an evening dose (300-400mg) to maintain steady levels throughout the day and avoid any mild digestive effects from a large single dose.
Start with 200-300mg of magnesium glycinate in the evening and assess your response over two weeks. Most women notice improved sleep within 3-5 days, better stress resilience within 1-2 weeks, and reduced hair shedding within 4-6 weeks as cortisol levels normalize and hair follicles re-enter the growth phase. If you don’t notice sleep improvements within two weeks, increase to 400mg in the evening.
Side effects are rare with glycinate or threonate, but some women experience mild drowsiness if they take too much too quickly. If this happens, reduce your dose and increase gradually. Loose stools are a sign you’ve exceeded your body’s absorption capacity; reduce the dose or switch to a form with slower release. And because magnesium can interact with certain medications (especially antibiotics, bisphosphonates, and some blood pressure medications), consult your doctor if you’re on prescription drugs.
For women dealing with hard water damage to hair and scalp, magnesium supplementation works synergistically with topical chelation. While a chelating shampoo like Regrowth+ removes the mineral buildup that blocks nutrient absorption at the scalp, magnesium supports the internal environment your follicles need to function optimally. You’re addressing the problem from both directions: external mineral removal and internal nutrient repletion.
Food Sources and Why They’re Not Enough
Whole food sources of magnesium include dark leafy greens (spinach, Swiss chard, kale), nuts and seeds (especially pumpkin seeds, almonds, and cashews), legumes (black beans, chickpeas), whole grains (quinoa, brown rice), dark chocolate (70% cacao or higher), and fatty fish (salmon, mackerel). These foods provide not just magnesium but also cofactors like vitamin B6 and zinc that enhance magnesium absorption and utilization.
But here’s the reality: even with a perfect diet, most women don’t consume enough magnesium to reach optimal levels. A study in Nutrition Reviews found that the average American woman consumes only 68% of the RDA for magnesium, and that’s before accounting for increased needs due to stress, hormonal fluctuations, or medication use. In the Gulf region, where access to fresh, magnesium-rich produce can be limited and expensive, and where dietary patterns often lean toward processed foods, the gap is even wider.
Soil depletion is another factor. Modern agricultural practices have reduced the magnesium content of crops by 25-80% compared to pre-industrial levels, according to research published in Journal of Food Composition and Analysis. Even if you’re eating spinach every day, you’re getting less magnesium per serving than your grandmother did from the same vegetable.
This doesn’t mean you should abandon food sources. A magnesium-rich diet provides the foundation, and the bioavailability of magnesium from whole foods is generally excellent because you’re getting it alongside other nutrients that enhance absorption. But for women with documented deficiency, chronic stress, sleep issues, or hair loss, food alone won’t close the gap quickly enough. Supplementation is necessary, and it should be paired with dietary improvation for best results.
The Gulf-Specific Magnesium Problem
If you’ve relocated to the Gulf region and noticed your sleep deteriorating, your stress levels rising, and your hair thinning, magnesium depletion is likely part of the picture. The environmental factors here create a perfect storm for deficiency.
Desalinated water, as mentioned earlier, contains virtually no magnesium. In contrast, natural groundwater in most parts of the world provides 10-50mg of magnesium per liter. If you’re drinking two liters of water per day, that’s a potential loss of 20-100mg of magnesium you’re not getting from your water supply. Over months and years, this adds up.
Heat exposure increases magnesium loss through sweat. Research shows that prolonged exposure to temperatures above 35°C (95°F) significantly increases urinary and sweat-based magnesium excretion. If you’re walking outside in 45°C heat, working out in hot conditions, or simply living in a climate where air conditioning is the only reprieve, you’re losing more magnesium than someone in a temperate climate.
The expat stress factor compounds everything. Relocation stress, professional pressure, social isolation, and the chronic low-level anxiety of adapting to a new environment all improve cortisol, which in turn depletes magnesium. A study in Psychoneuroendocrinology found that individuals undergoing major life transitions had significantly lower intracellular magnesium levels and higher cortisol compared to stable control groups. For women in the Gulf, this isn’t theoretical. It’s measurable, and it’s affecting your sleep and your hair.
References
- The Effects of Magnesium Supplementation on Subjective Anxiety and Stress, A Systematic Review - Nutrients, PubMed
- Magnesium in Prevention and Therapy - Nutrients, PubMed Central
- The effect of magnesium supplementation on primary insomnia in elderly: A double-blind placebo-controlled clinical trial - Journal of Research in Medical Sciences, PubMed
- Magnesium-L-threonate prevents and restores memory deficits associated with neuropathic pain - Neuropharmacology, PubMed
- Suboptimal magnesium status in the United States: are the health consequences underestimated? - Nutrition Reviews, PubMed
