You’re three weeks postpartum, and you can’t remember the last time you ate a proper meal. Between nursing every two hours and the relentless heat making you feel constantly drained, you’ve been surviving on whatever you can grab with one hand. Your hair is coming out in clumps when you shower, your skin looks dull despite the humidity, and you’re so tired you could cry. Everyone says this is normal. But here’s what they’re not telling you: your body’s nutritional needs in the Gulf after giving birth are dramatically different from what standard postpartum advice assumes.
The combination of breastfeeding, recovery from delivery, extreme heat, and the unique challenges of desalinated water creates a perfect storm of nutritional deficiency that most new mothers don’t see coming. This article contains affiliate links. See our affiliate disclosure for details. Medically reviewed by Dr. Layla Hassan, Trichologist.
The standard postpartum nutrition advice you’ll find online was written for temperate climates with different water quality and environmental stressors. When you’re living in 45-degree heat, drinking desalinated water, and losing fluids through both nursing and constant perspiration, those guidelines fall dangerously short. Let’s look at what your body actually needs right now.
The Hydration Crisis Nobody Warns You About
Standard breastfeeding advice tells you to drink eight glasses of water a day. That’s baseline hydration for a temperate climate. In the Gulf, you’re losing fluids through three channels simultaneously: milk production, perspiration in extreme heat, and the dehydrating effect of air conditioning cycling you between temperature extremes. Research from the World Health Organization shows breastfeeding mothers need an additional 700-1000ml of fluids daily, but that’s before accounting for environmental factors.
Here’s what actually happens. You produce roughly 750ml of breast milk daily in the early months. In 45-degree heat, you’re losing another 1-2 liters through perspiration, even indoors. Your baseline hydration need jumps from 2 liters to nearly 4 liters daily, and most women aren’t coming close to that. The first sign isn’t thirst. It’s that your milk supply dips in the afternoon, your urine turns dark yellow, and you feel exhausted in a way that sleep doesn’t fix.
The type of water matters too. Desalinated water, common across the Gulf, lacks the natural mineral content your body expects. You’re drinking more but absorbing less. Desalinated water’s effect on mineral absorption means you need to actively replenish electrolytes, not just volume. Add a pinch of sea salt to your water, or drink coconut water between nursing sessions. Your body needs sodium, potassium, and magnesium to actually use the water you’re consuming.
Set a timer. Every two hours, drink a full glass of water, whether you feel thirsty or not. Keep a large water bottle next to your nursing station. By the time you feel thirsty in this climate, you’re already significantly dehydrated.
 Breastfeeding mothers in extreme heat need significantly more fluids than standard recommendations suggest.
Breastfeeding mothers in extreme heat need significantly more fluids than standard recommendations suggest.
Iron Deficiency: The Invisible Drain
You lost blood during delivery. If you’re breastfeeding, you’re not menstruating, which sounds like a break, but your iron stores are still depleted from pregnancy and birth. A 2019 study in the Journal of Perinatal Medicine found that 50% of postpartum women have depleted iron stores by six weeks, even without obvious anemia. In the Gulf, that number is likely higher because the heat increases your blood volume needs.
Low iron doesn’t just make you tired. It’s directly connected to postpartum hair loss that seems worse than it should be. Your hair follicles are among the first systems your body will sacrifice when resources are scarce. If you’re losing more hair than expected, or it’s not growing back by six months postpartum, check your ferritin levels, not just hemoglobin.
The standard postpartum iron supplement (if you’re even taking one) is often too little, too late. You need 27mg of elemental iron daily while breastfeeding, preferably in ferrous bisglycinate form, which is gentler on your stomach. Take it with vitamin C to improve absorption. Orange juice works, but a supplement is more reliable. Don’t take iron with tea, coffee, or calcium supplements, as they block absorption.
Get your levels tested at six weeks postpartum. Ask specifically for ferritin (stored iron), not just hemoglobin. Ferritin below 30 ng/mL will cause hair loss and fatigue, even if your hemoglobin looks normal. Most doctors won’t test ferritin unless you ask.
The Vitamin D Paradox
You live in one of the sunniest regions on Earth, yet vitamin D deficiency is epidemic among Gulf residents, especially new mothers. The counterintuitive reality of vitamin D deficiency in sun-heavy climates comes down to behavior: you avoid the sun because it’s dangerously hot, you wear sun protection when you do go out, and you spend most of your time in air-conditioned spaces.
Pregnancy depletes your vitamin D stores. Breastfeeding depletes them further because you’re passing vitamin D to your baby through milk. If you’re not supplementing, you’re running on empty. Research published in Nutrients shows that 60-80% of breastfeeding mothers in the Gulf region have insufficient vitamin D levels, defined as below 30 ng/mL.
Low vitamin D doesn’t just affect your bones. It’s linked to postpartum depression, immune dysfunction, and chronic fatigue. It also affects your baby’s development if you’re breastfeeding. The standard 400 IU supplement most prenatal vitamins contain is nowhere near enough. You need 2000-4000 IU daily while nursing, and your baby needs a separate infant supplement.
Get tested. Don’t assume you’re fine because you live in a sunny climate. If your level is below 30 ng/mL, your doctor may recommend a loading dose before switching to maintenance. Take vitamin D with a meal containing fat, as it’s fat-soluble and won’t absorb properly on an empty stomach.
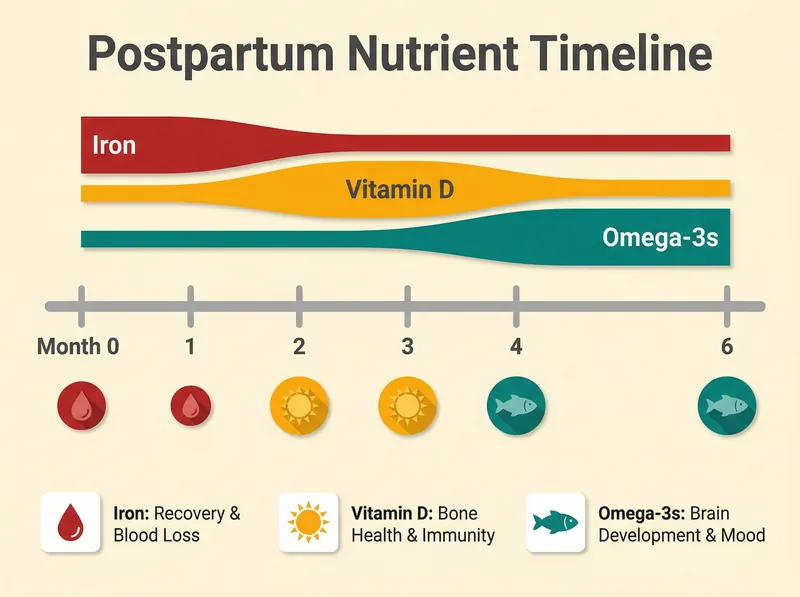 Your body’s nutritional priorities shift significantly in the months after delivery.
Your body’s nutritional priorities shift significantly in the months after delivery.
Omega-3s for Your Brain and Your Baby’s
DHA, an omega-3 fatty acid, is critical for your baby’s brain development and your own mental health. Your stores were depleted during pregnancy, when your baby was literally building a brain using your DHA reserves. If you’re breastfeeding, you’re continuing to transfer DHA through milk. A study in Prostaglandins, Leukotrienes and Essential Fatty Acids found that maternal DHA levels drop by 50% during pregnancy and don’t recover without supplementation.
Low omega-3s are linked to postpartum mood disorders. That brain fog, irritability, and emotional fragility you’re feeling isn’t just sleep deprivation. Your brain needs fat to function, specifically DHA. If you’re not eating fatty fish twice a week or taking a supplement, you’re running on fumes.
The problem in the Gulf is that fresh, high-quality fish can be expensive and hard to source consistently. Frozen fish loses some omega-3 content. Most women aren’t getting anywhere near the 200-300mg of DHA daily recommended for breastfeeding mothers. A high-quality fish oil or algae-based supplement is the most reliable solution.
Choose a supplement with at least 200mg DHA per serving. Algae-based options work if you’re vegetarian. Take it with food to avoid fishy aftertaste and improve absorption. Your baby’s brain is developing rapidly in the first year, and your mental clarity matters too.
The Mineral Depletion You Can’t See
Magnesium, zinc, and calcium are quietly depleted during pregnancy and breastfeeding, and the Gulf environment makes it worse. Magnesium is lost through sweat, and you’re sweating constantly. Zinc is transferred to your baby through milk. Calcium is pulled from your bones if your diet doesn’t provide enough. Research in the Journal of Trace Elements in Medicine and Biology shows that lactating women lose significant amounts of these minerals daily.
Low magnesium causes muscle cramps, insomnia, and anxiety. Low zinc affects your immune system and wound healing, which matters if you had a C-section or tearing. Low calcium increases your risk of bone density loss, which becomes a problem years later. These deficiencies are silent until they’re not.
The challenge is that desalinated water doesn’t contain the trace minerals that natural water sources provide. You’re drinking more water but getting fewer minerals. Your diet needs to compensate. Dark leafy greens, nuts, seeds, and whole grains provide magnesium. Red meat and shellfish provide zinc. Dairy and fortified plant milks provide calcium.
If you’re taking a postnatal multivitamin, check the mineral content. Many are heavy on vitamins but light on minerals. You may need a separate magnesium supplement (300-400mg daily) and a zinc supplement (15-20mg daily). Take magnesium at night as it can help with sleep.
Protein: The Foundation You’re Probably Missing
You need significantly more protein while breastfeeding, roughly 25 grams more per day than your pre-pregnancy baseline. That’s about 70-80 grams daily for most women. A review in Nutrients found that inadequate protein intake during lactation affects milk composition, maternal recovery, and long-term metabolic health.
Here’s the reality: you’re probably not eating enough. A piece of chicken breast is about 25 grams. Two eggs are 12 grams. A cup of lentils is 18 grams. To hit 70-80 grams, you need protein at every meal and most snacks. When you’re exhausted and overwhelmed, protein is usually the first thing to drop from your diet because it requires preparation.
Protein isn’t just about milk production. It’s about your hair, skin, wound healing, and energy levels. Hair loss that won’t stop is often a combination of iron deficiency and inadequate protein. Your body will always prioritize vital functions over hair growth, and hair is expendable when resources are tight.
Make it easy. Keep hard-boiled eggs in the fridge. Buy pre-cooked rotisserie chicken. Use protein powder in smoothies (whey or plant-based, both work). Greek yogurt, cheese, nuts, and hummus are grab-and-go options. You don’t need perfect meals. You need consistent protein intake throughout the day.
What About Your Scalp and Hair?
Postpartum hair loss is normal, but the Gulf environment makes it worse. The combination of nutritional depletion, hormonal shifts, hard water, and heat stress creates a perfect storm. By three to six months postpartum, you’re likely shedding significantly more than you did before pregnancy. This is telogen effluvium, a stress-induced shedding phase triggered by the hormonal drop after delivery.
What’s not normal is hair that won’t grow back, or shedding that continues past six months. That’s usually a sign of underlying nutritional deficiency, particularly iron, protein, or zinc. Your scalp health is a direct reflection of your internal nutritional state. If your scalp feels dry, itchy, or inflamed, your body is telling you something.
Hard water makes everything worse. The mineral deposits in Gulf water coat your hair and scalp, making it harder for topical treatments to work and creating buildup that can clog follicles. A chelating shampoo like Regrowth+ can help remove that buildup, but the real solution is internal. You can’t out-supplement a bad diet, but you also can’t out-eat bad water quality. You need both.
Focus on nutrition first. Hair is a long game. What you eat today affects the hair that grows three months from now. If you’re addressing deficiencies now, you should see improvement by six to nine months postpartum. If you’re not seeing improvement by then, get your levels tested again.
References
- Infant and young child feeding - World Health Organization
- Iron deficiency and anemia in pregnancy and postpartum period - Journal of Perinatal Medicine
- Vitamin D Status and Its Adequacy in Healthy Danish Perimenopausal Women - Nutrients (via PubMed Central)
- Maternal DHA supplementation and pregnancy outcomes - Prostaglandins, Leukotrienes and Essential Fatty Acids
- Trace elements in lactation - Journal of Trace Elements in Medicine and Biology
- Protein Requirements During Pregnancy and Lactation - Nutrients (via PubMed Central)
