You’ve been managing everything. The international move, the new role, the climate adjustment, the cultural adaptation. You’re handling it. But your skin is telling a different story.
The breakouts that won’t respond to your usual products. The dullness that no amount of vitamin C seems to fix. The fine lines that appeared seemingly overnight, or the redness that flares unpredictably. These aren’t random skin problems. They’re your body’s visible response to chronic stress, and they’re being amplified by environmental factors you might not have connected.
This article contains affiliate links. See our affiliate disclosure for details.
Medically reviewed by Dr. Layla Hassan, Trichologist. The relationship between chronic stress and skin inflammation is well-documented in dermatological research. When you’re under sustained pressure, your body releases cortisol and other stress hormones that directly affect skin barrier function, oil production, and inflammatory responses. In dry, hard water climates, these effects compound. The environmental stressors that affect your hair and scalp are simultaneously compromising your skin’s ability to recover from stress-induced damage.
Key Takeaways
• Chronic stress triggers cortisol release that increases oil production, breaks down skin barrier function, and promotes inflammation, leading to acne, premature aging, and sensitivity.
• Environmental factors in arid climates (hard water, extreme heat, low humidity, indoor AC) compound stress-related skin damage by further compromising barrier function and hydration.
• Stress-related skin changes typically appear 2-4 weeks after sustained high-stress periods, making the connection easy to miss without tracking patterns.
• Breaking the stress-skin cycle requires addressing both internal cortisol management (sleep, nutrition, stress reduction) and external barrier protection (gentle cleansing, strategic hydration, mineral management).
• Recovery is possible but takes 6-12 weeks of consistent intervention, as skin barrier repair and hormonal rebalancing both require sustained effort over time.
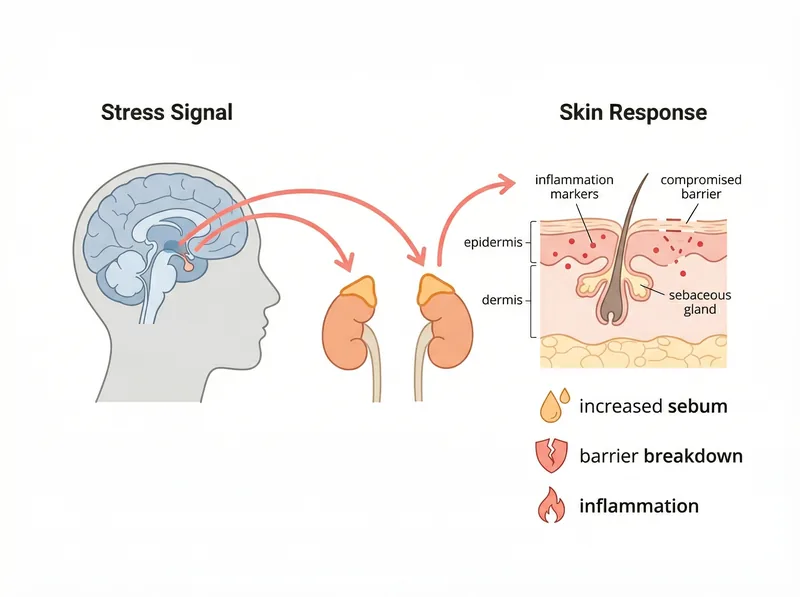 The stress response triggers a cascade of hormonal changes that directly affect skin barrier function, oil production, and inflammation levels.
The stress response triggers a cascade of hormonal changes that directly affect skin barrier function, oil production, and inflammation levels.
The Cortisol-Skin Connection: What’s Actually Happening
When you’re stressed, your hypothalamus signals your pituitary gland, which triggers your adrenal glands to release cortisol. This is the stress response you’ve heard about. What you might not know is that your skin has cortisol receptors. It’s not just experiencing the downstream effects of stress. It’s a direct target.
Research published in the International Journal of Molecular Sciences shows that improved cortisol levels increase sebum production by up to 60% in some individuals. That’s not a small uptick. It’s enough to shift your skin from balanced to actively breaking out, especially if you’re already dealing with the occlusive effects of mineral-heavy water.
But increased oil is just one piece. Cortisol also breaks down collagen and elastin, the structural proteins that keep your skin firm and resilient. It suppresses your skin’s production of hyaluronic acid, which means your skin holds less water. And it triggers inflammatory pathways that show up as redness, sensitivity, and a compromised barrier that can’t protect itself from environmental damage.
The timeline matters here. You won’t see these changes immediately after a stressful day. The visible effects typically appear 2-4 weeks after sustained stress begins, which is why it’s easy to miss the connection. By the time your skin is reacting, you might have moved past the stressor mentally, making it seem like your skin is breaking out for no reason.
How Anxiety Changes Your Skin’s Behavior
Chronic anxiety creates a state of sustained physiological arousal that affects skin in ways distinct from acute stress. Your nervous system stays activated, which means inflammatory markers remain improved even when you’re not consciously feeling anxious. The American Academy of Dermatology notes that this chronic low-grade inflammation accelerates cellular aging and impairs wound healing, which is why stress-related breakouts take longer to resolve.
Anxiety also changes your skin’s circadian rhythm. Your skin has its own biological clock that governs when it repairs damage, produces new cells, and maintains barrier function. These processes happen primarily at night. When anxiety interferes with sleep quality or keeps cortisol improved into evening hours, your skin misses its repair window. You wake up looking tired because your skin literally didn’t complete its maintenance cycle.
There’s a behavioral component too. Anxiety increases unconscious face-touching, picking, and rubbing. You might not realize you’re doing it, but studies tracking these behaviors show that anxious individuals touch their faces up to 16 times per hour, compared to 3-4 times for baseline populations. Each touch transfers bacteria, changes healing, and can introduce environmental irritants directly into compromised areas.
The gut-skin-brain axis adds another layer. Anxiety alters gut microbiome composition, which affects systemic inflammation levels that show up on your skin. This is why stress-related skin issues often coincide with digestive changes. They’re both manifestations of the same underlying nervous system dysregulation.
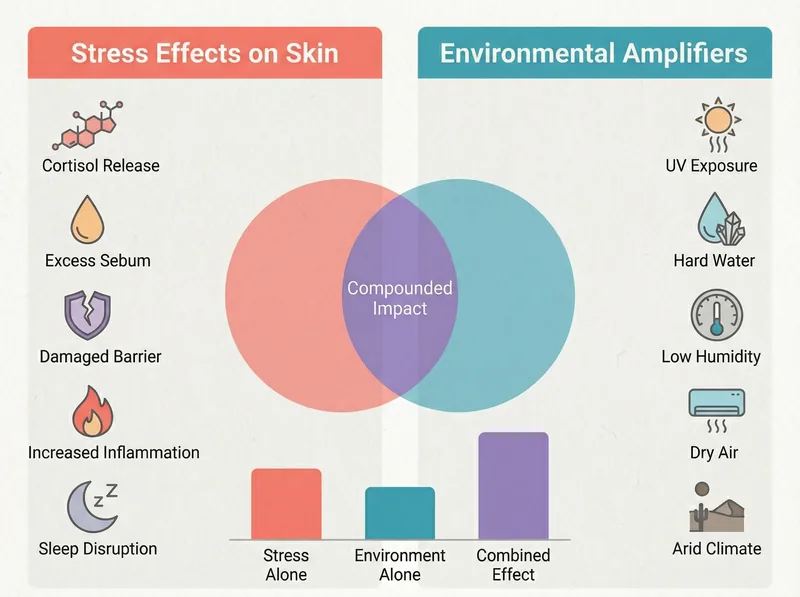 Environmental factors in arid regions create a perfect storm for stress-related skin issues, compounding the effects of cortisol on barrier function.
Environmental factors in arid regions create a perfect storm for stress-related skin issues, compounding the effects of cortisol on barrier function.
Environmental Amplifiers: Why It’s Worse Here
If you’ve relocated to a dry, hard water climate, your stress-related skin problems are likely more severe than they were in your previous environment. This isn’t coincidental. The environmental factors that make this region challenging for hair and scalp health create the same compounding effects for facial skin.
Hard water contains high concentrations of calcium and magnesium that bind to your skin’s surface, creating a film that prevents proper hydration and makes cleansing less effective. When your skin barrier is already compromised by cortisol, this mineral layer acts like a seal that traps inflammation and prevents recovery. You’re trying to heal, but the water you’re washing with is actively working against you.
The extreme heat and low humidity create additional challenges. When ambient humidity drops below 30% (common in arid regions), your skin loses moisture faster than it can produce it, regardless of how much water you drink. Research on transepidermal water loss shows that this effect is exponential. At 50% humidity, skin maintains reasonable hydration. At 20% humidity, water loss increases by 300-400%.
Indoor air conditioning provides relief from heat but further drops humidity levels, often to 10-15% in heavily cooled spaces. If you’re spending 8-10 hours a day in an air-conditioned office, your skin is experiencing desert-level dryness for most of your waking hours. Cortisol has already impaired your barrier function. The environment is ensuring it can’t recover between stress episodes.
This creates a feedback loop. Environmental stress on your skin triggers inflammatory responses that your body interprets as another stressor, releasing more cortisol, which further damages your barrier, making you more vulnerable to environmental damage. Breaking this cycle requires addressing both the internal hormonal component and the external environmental factors simultaneously.
Identifying Stress-Related Skin Changes
Stress-induced skin problems have characteristic patterns that distinguish them from other causes. The most common manifestation is adult acne that appears primarily along the jawline, chin, and lower cheeks. This distribution corresponds to areas with high concentrations of hormone-responsive sebaceous glands. If you’re breaking out in a beard pattern (even if you don’t have a beard), cortisol is likely involved.
Premature aging is another hallmark. Fine lines appearing around your eyes, forehead, and mouth that seem disproportionate to your age are often stress-related. Mayo Clinic research indicates that chronic stress can accelerate cellular aging by 9-17 years at the chromosomal level, which manifests visibly as premature wrinkling and loss of elasticity.
Increased sensitivity is a red flag. If products you’ve used for years suddenly cause stinging, burning, or redness, your barrier function has been compromised. Stress-induced barrier breakdown makes your skin reactive to ingredients it previously tolerated, including gentle actives like niacinamide or even fragrance-free moisturizers.
Uneven texture and dullness signal impaired cellular turnover. When cortisol changes your skin’s repair cycle, dead cells accumulate on the surface instead of shedding naturally. This creates a rough, lackluster appearance that doesn’t improve with exfoliation alone. The problem isn’t the dead cells. It’s that your skin isn’t producing healthy new cells efficiently.
Redness and inflammation that fluctuates with your stress levels is perhaps the clearest indicator. If you notice your skin looks inflamed after difficult work weeks or calms during vacation, you’re seeing the direct cortisol-inflammation connection in real time.
Breaking the Cycle: Internal Interventions
Addressing stress-related skin damage requires working from the inside out. Topical treatments alone won’t resolve problems driven by sustained cortisol improvion. You need to interrupt the hormonal cascade.
Sleep is non-negotiable. Studies on sleep deprivation and skin function show that even one night of poor sleep increases inflammatory markers and impairs barrier recovery by up to 30%. Chronic sleep changeion compounds these effects exponentially. If you’re getting less than 7 hours consistently, your skin can’t complete its repair processes regardless of what products you use.
The connection between sleep quality and cortisol regulation is direct. Poor sleep keeps cortisol improved into evening hours when it should naturally decline, preventing your body from entering the parasympathetic state necessary for tissue repair. Prioritizing sleep isn’t self-care. It’s a biological requirement for skin recovery.
Nutrition plays a more significant role than most people realize. Chronic stress depletes specific micronutrients that your skin needs for barrier function and inflammation control. Magnesium, B vitamins, vitamin C, and omega-3 fatty acids are all consumed at higher rates during sustained stress. Strategic supplementation can help, but whole food sources are more effective for most people.
Adaptogenic herbs like ashwagandha and rhodiola have evidence supporting their ability to modulate cortisol responses, though the research is still emerging. What’s clearer is that consistent stress management practices, whether meditation, exercise, or therapy, measurably reduce inflammatory markers within 6-8 weeks of regular practice.
Hydration deserves specific attention in dry climates. Your water needs increase significantly in hot, arid environments, and dehydration amplifies cortisol’s negative effects on skin. But drinking more water alone won’t fix stress-related skin problems if the underlying hormonal dysregulation isn’t addressed.
External Protection: Managing Environmental Factors
While you’re working on internal cortisol management, you need to protect your skin from environmental factors that compound stress-related damage. In hard water regions, this starts with how you cleanse.
Switch to a gentle, pH-balanced cleanser that won’t strip your already compromised barrier. Avoid sulfates (sodium lauryl sulfate, sodium laureth sulfate) which are particularly harsh in hard water. Look for cleansers with added chelating agents like EDTA or citric acid that help prevent mineral buildup. A chelating shampoo like Regrowth+ works for scalp care, and the same principle applies to facial cleansing, though you’ll want a formula specifically designed for facial skin’s thinner, more delicate structure.
Consider installing a shower filter or using filtered water for your final rinse. While shower filters can’t remove all minerals, they can reduce chlorine and some heavy metals that further irritate stressed skin. The impact of hard water on skin barrier function is measurable, and reducing exposure helps your skin recover faster.
Moisturizer strategy needs to change in dry climates. You need both humectants (to draw water into skin) and occlusives (to prevent water loss). Hyaluronic acid, glycerin, and urea are effective humectants, but they need to be sealed in with ceramides, squalane, or shea butter. In low humidity environments, humectants alone can actually increase water loss by drawing moisture from deeper skin layers when there’s no atmospheric moisture to pull from.
Sunscreen is critical but complicated. Stress-compromised skin often reacts to chemical sunscreen filters. Mineral sunscreens (zinc oxide, titanium dioxide) are generally better tolerated but can leave a white cast that’s socially unacceptable in professional settings. Finding sunscreens that work in extreme heat without white cast requires testing, but it’s worth the effort. UV exposure increases cortisol production, creating another feedback loop you need to interrupt.
Indoor humidity control helps more than most people expect. A small humidifier in your bedroom can increase ambient humidity to 40-50% during sleep hours, which is when your skin does most of its repair work. This isn’t a cure, but it removes one environmental barrier to recovery.
What Recovery Actually Looks Like
Managing expectations is important. Stress-related skin damage doesn’t resolve quickly, even with perfect intervention. Your skin barrier takes 28-45 days to fully regenerate under ideal conditions. When it’s been compromised by sustained cortisol improvion and environmental stress, recovery takes longer.
You’ll typically see initial improvements in 2-3 weeks: reduced inflammation, fewer new breakouts, less sensitivity. But full recovery of barrier function, texture, and resilience takes 6-12 weeks of consistent intervention. This timeline assumes you’re addressing both internal hormonal factors and external environmental protection simultaneously.
Some people see their skin get slightly worse before it improves, particularly if they’re introducing new products or changing their cleansing routine. This isn’t necessarily a bad sign. It can indicate that trapped inflammation is being released as your barrier begins to normalize. But if worsening continues beyond 10-14 days, reassess your approach.
Relapse is common when stress levels spike again. Your skin will likely react faster and more severely to future stress episodes once it’s been sensitized. This isn’t failure. It’s your skin’s adapted response pattern. The goal isn’t to make your skin stress-proof. It’s to reduce the severity and duration of stress-related flares through faster intervention.
Professional support can accelerate recovery. A dermatologist can assess whether you need prescription intervention for severe acne or inflammation. A therapist can help with stress management techniques that reduce cortisol more effectively than self-directed approaches. There’s no shame in needing support. Chronic stress is a physiological condition that often requires professional treatment.
References
- The Impact of Psychological Stress on Skin Function - PubMed - International Journal of Molecular Sciences
- Stress and Skin: An Overview of Mind Body Therapies as a Treatment Strategy in Dermatology - PubMed Central
- How Stress Affects Your Skin - American Academy of Dermatology
- Sleep Deprivation and Skin Barrier Function - PubMed
- Transepidermal Water Loss in Low Humidity Environments - PubMed Central
